Most people do not need a dental implant after wisdom tooth removal because third molars rarely serve essential chewing or alignment roles. If a wisdom tooth is removed and you want to restore chewing function or prevent localized bone loss in that specific spot, an implant is technically possible but usually unnecessary.
This post will help you weigh why extraction often suffices, when an implant becomes a sensible option, and how that decision ties into your long-term oral health and treatment planning. Expect clear guidance on how removal affects your mouth, what replacement choices look like, and what to consider when planning for the future.
Understanding Wisdom Tooth Removal
You will learn why dentists remove wisdom teeth, what to expect during healing, and the complications to watch for after surgery. The following explains the signs that lead to extraction, typical recovery steps, and warning signs that need prompt attention.
Reasons for Wisdom Tooth Extraction
Dentists remove wisdom teeth when they cause pain, infection, or threaten surrounding teeth. Common reasons include impaction (tooth trapped in bone or gum), crowding that shifts nearby teeth, decay in a partially erupted tooth, and recurrent pericoronitis (gum infection around the tooth).
You may also have extraction recommended before orthodontic work or radiation therapy to the head and neck.
Your dentist will evaluate X‑rays, bite alignment, and symptoms before recommending removal. If a wisdom tooth is fully erupted, healthy, and functional, your provider often leaves it in place. Extraction becomes more likely when the tooth poses a measurable risk to oral health.
Healing and Recovery Process
Expect bleeding for the first 24 hours, with a blood clot forming in the socket within a day. You will have swelling and pain that peak around 48–72 hours; use prescribed or over‑the‑counter analgesics and cold packs to manage symptoms.
Eat soft foods, avoid straws and smoking for at least one week, and keep the mouth gently clean—saltwater rinses typically begin 24 hours after surgery.
Stitches may be dissolvable and usually fall out or dissolve within 7–10 days. Most people return to normal activities within 3–5 days, but full bone and soft‑tissue healing can take several weeks to months. Follow postoperative instructions and attend any follow‑up appointments.
Potential Complications
Dry socket (alveolar osteitis) occurs when the clot dislodges, causing intense pain 3–5 days after extraction; it requires prompt dental care. Infection, prolonged numbness from nerve irritation (mental or inferior alveolar nerve), and excessive bleeding are other possible complications.
Less common risks include damage to adjacent teeth, sinus communication after upper molar removal, and delayed healing in smokers or people with certain medical conditions.
Contact your dentist if you have fever, uncontrolled bleeding, severe swelling that worsens after 72 hours, persistent numbness beyond a few days, or worsening pain not relieved by medication. Early intervention lowers the chance of long‑term problems.
Dental Implant Options After Extraction
You can often replace a removed wisdom tooth with an implant, a bridge, or leave the space as is depending on function and bone health. Decisions center on your jawbone quality, oral health risks, and how the missing tooth affects chewing or nearby teeth.
Evaluating Candidacy for Implants
You need sufficient jawbone height and width where the tooth was removed. Your dentist will use a clinical exam and a CBCT or periapical X-ray to measure bone volume and check for proximity to nerves or the sinus.
Healthy gum tissue and absence of active infection matter. Uncontrolled diabetes, heavy smoking, or recent radiation to the head/neck raise failure risk and may require medical clearance or modification of the treatment plan.
Your bite and neighboring teeth influence whether an implant is appropriate. If adjacent teeth have shifted or you have severe malocclusion, orthodontic or restorative steps may be needed first. Expect discussion of costs, timelines, and alternative options like bridges or removable partials.
Types of Dental Implants
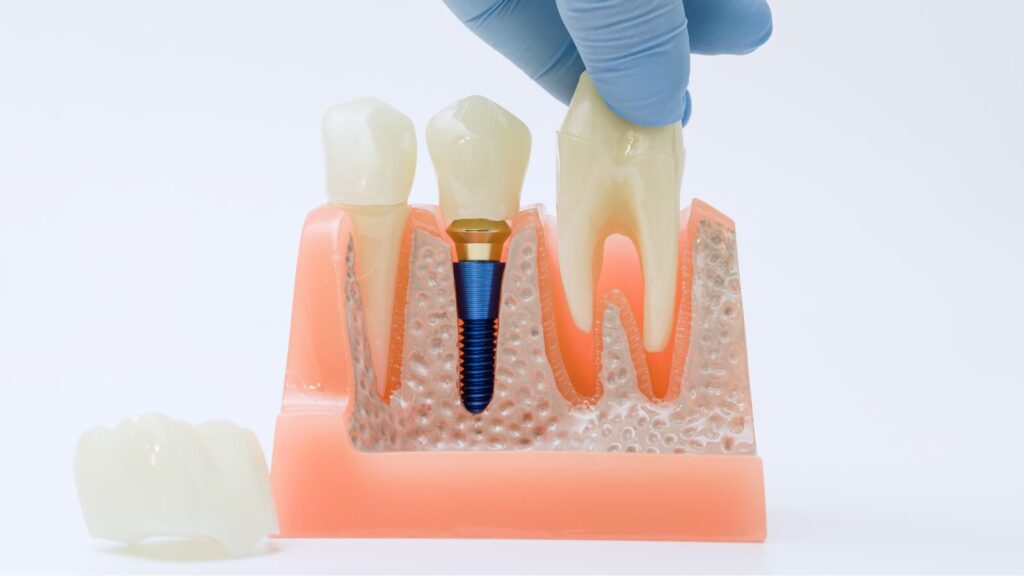
Endosseous (root-form) titanium implants are the standard choice; they act as an artificial root and integrate with bone. Zirconia implants exist as a metal-free alternative for patients with metal sensitivities or specific aesthetic needs.
Single crowns attach to one implant for an isolated gap. If multiple adjacent teeth are missing, you may get two implants supporting a bridge or an implant-retained removable denture for larger spans. Abutments can be stock or custom; custom abutments often give better emergence profile and soft-tissue support.
Surface coatings and implant designs vary to promote faster osseointegration or better primary stability. Your clinician will recommend a specific system based on bone quality, location (lower vs upper jaw), and long-term prosthetic goals.
Timing for Implant Placement
Immediate placement occurs at the time of extraction when bone is intact and there is no infection. This shortens treatment time but requires good primary stability and favorable socket anatomy.
Delayed placement happens after 8–12 weeks of healing when soft tissue closes and initial bone remodeling occurs. This approach reduces infection risk and may be chosen when the socket anatomy is compromised.
Staged placement with bone grafting may take several months: grafting first, then waiting 3–6 months for graft consolidation before placing the implant. Your dentist will select timing based on infection status, bone loss, and whether you need ridge preservation or augmentation.
Preparing for Long-Term Oral Health
Plan for preserving jaw structure, controlling gum inflammation, and understanding costs so future implant options remain viable and predictable.
Bone Preservation Techniques
After extraction, bone resorption begins quickly; you should act to preserve ridge height if you plan implants later. Your surgeon can place a bone graft into the socket immediately (socket preservation) using materials such as autograft, allograft, xenograft, or synthetic grafts to limit vertical and horizontal bone loss.
If extraction is delayed or infection is present, consider a staged approach: first resolve infection, then graft or perform ridge augmentation once soft tissues are healthy.
Monitor healing with 3–6 month radiographic checks so your team can time implant placement when bone volume is adequate.
Ask about guided bone regeneration (membrane and graft combination) for larger defects and consider a cone-beam CT (CBCT) scan to measure width and height precisely before implant planning.
Maintaining Gum Health
Healthy peri-implant tissues start with healthy gums now. You must maintain daily plaque control—twice-daily brushing with a soft brush and interdental cleaning (floss, interdental brushes, or water flosser) focused on molar regions where wisdom teeth sat.
Schedule professional cleanings every 3–6 months based on your periodontal status; your hygienist will remove subgingival calculus and monitor pocket depths.
If you have history of periodontitis, expect more frequent maintenance and targeted antimicrobials (chlorhexidine rinse short-term or locally delivered antibiotics) to reduce bacterial load before implant placement.
Stop smoking and control diabetes; both significantly increase risk of implant failure and slow gum healing.
Cost Considerations
Plan financially for staged care: extraction, possible grafting, CBCT imaging, implant placement, abutment, and crown each carry separate fees.
Ask for an itemized estimate and payment timeline; many practices offer phased billing so you pay for extraction and grafting first, then implant surgery months later.
Check whether your insurance covers extractions or grafts—coverage for implants is often limited—so verify benefits and preauthorization requirements.
Evaluate financing options (medical credit, dental financing plans) and get a written treatment plan that lists implant brand and expected timeline to avoid unexpected costs.
