You want a durable, comfortable solution for missing teeth—not a short-term bargain that leads to higher costs and more complications later. Low-cost implant offers may reduce the upfront price, but they can increase the risk of implant failure, infection, additional surgeries, and progressive bone loss that becomes far more expensive over time.
This article explains how hidden long-term expenses, medical risks, and overall oral health consequences compare to the initial price tag. You’ll learn what red flags to watch for when evaluating treatment offers and why investing in quality planning, materials, and surgical expertise protects both your smile and your finances. If you are considering a full-arch solution, exploring full mouth dental implants in Woodbury, MN can help you understand how advanced techniques and experienced care contribute to long-term stability and value.
Hidden Long-Term Costs of Cheap Dental Implants
Choosing low-cost implants often leads to recurring work, more invasive corrective procedures, and bills you didn’t plan for. Expect higher maintenance, extra surgeries, and surprise expenses that can exceed the initial savings.
Frequent Repairs and Replacements
Cheap implant components and lower-grade materials increase the chance you’ll need repairs or replacements. You may face loose abutments, fractured crowns, or implant body failure within a few years rather than decades.
Each repair requires professional time, lab fees, and new parts. That can mean multiple visits for adjustments, temporary crowns, and eventual full component replacement. If the implant fails, removal and site rehabilitation add substantial costs.
Replacement also often involves more complex procedures than the original placement. You could need bone grafting or sinus lifts before a new implant can be placed, further increasing expense and recovery time.
Additional Dental Procedures
Substandard implants raise the risk of complications that necessitate further dentistry. Peri-implantitis (infection and bone loss around the implant) can require deep cleaning, antibiotics, and surgical debridement.
If bone or soft tissue is lost, expect grafting, membrane placement, or soft-tissue grafts to restore the site. Those procedures add material costs and specialist fees, and they extend treatment timelines by months.
When infection or mechanical failure occurs, you may need implant removal, ridge preservation, and repeat implant placement. Each step multiplies costs and exposes you to additional surgical risk.
Unexpected Out-of-Pocket Expenses
Low advertised prices often exclude diagnostics and follow-up care. You may pay separately for CT scans, lab work, surgical guides, temporary prosthetics, and anesthesia.
Travel for bargain clinics (domestic or abroad) adds lodging and transportation costs. If complications arise after returning home, local dentists may charge premium rates to manage work they did not perform originally.
Insurance and warranties can be limited or voided by cheaper implant systems and non-accredited providers. That leaves you personally responsible for long-term monitoring, emergency visits, and corrective treatments.
Risks and Complications From Low-Cost Implants
Choosing a low-cost implant can lead to mechanical failure, compromised materials, and higher infection risk that often require additional surgeries, prolonged treatment, and extra expense. These issues affect bone health, adjacent teeth, and long-term function.
Implant Failure and Removal
If an implant doesn’t osseointegrate (bond) with your jawbone, it may loosen or tilt within months. Failure can come from poor surgical technique, insufficient bone volume, or skipping necessary bone grafts.
Removal causes added surgery, greater bone loss, and a need for grafting before you can retry implantation. That extends healing time and increases costs for anesthesia, clinic time, and new components.
Repeated attempts reduce available bone and raise the chance of visible gum recession or implant loss near sinuses or nerves. Expect higher cumulative expense and longer time without a stable tooth replacement.
Poor Quality Materials Used
Low-cost providers sometimes use off-brand or inferior-grade titanium or zirconia that show inconsistent tolerances. Components with poor fit create micro-gaps where bacteria accumulate and mechanical stress concentrates.
Substandard abutments and crowns wear faster, fracture, or strip screws, forcing early replacement. You may face additional lab fees and chair time for remakes.
Non-medical-grade alloys can cause local irritation or accelerated corrosion. That undermines long-term stability and may necessitate full-system replacement with certified parts, which costs significantly more than choosing quality materials initially.
Increased Likelihood of Infection
When providers cut corners on sterility, pre-op imaging, or surgical planning, your risk of peri-implant infection rises. Infections present as pain, swelling, drainage, or progressive bone loss around the implant.
Treating infection often requires antibiotics, debridement, and sometimes implant removal followed by bone grafting. Each step adds expense and delays restoring function.
Early detection matters: you should expect follow-up imaging and probing. If those are omitted in low-cost settings, infections can become chronic and harder to resolve, increasing the probability of permanent implant loss.
Impact on Oral Health and Overall Wellbeing
Cheap implants can lead to predictable problems that affect jaw structure, chewing efficiency, appearance, and speech. These problems often require additional treatment and can worsen general health if left unaddressed.
Bone Loss and Gum Recession
If an implant lacks proper fit, surface quality, or precise placement, your jawbone may not receive the normal mechanical stimulation that preserves bone volume. Over time this leads to progressive bone resorption around the implant and adjacent teeth, increasing the risk of implant loosening or failure.
Gum recession often accompanies bone loss. Exposed implant components or threads create areas that trap plaque and irritate soft tissue, raising your chance of peri-implantitis — an infection-driven inflammation that accelerates bone loss.
Treatments for advanced bone and soft-tissue loss are complex. You may need bone grafts, guided bone regeneration, or soft-tissue grafting, all of which increase cost, extend healing time, and complicate future restorative options.
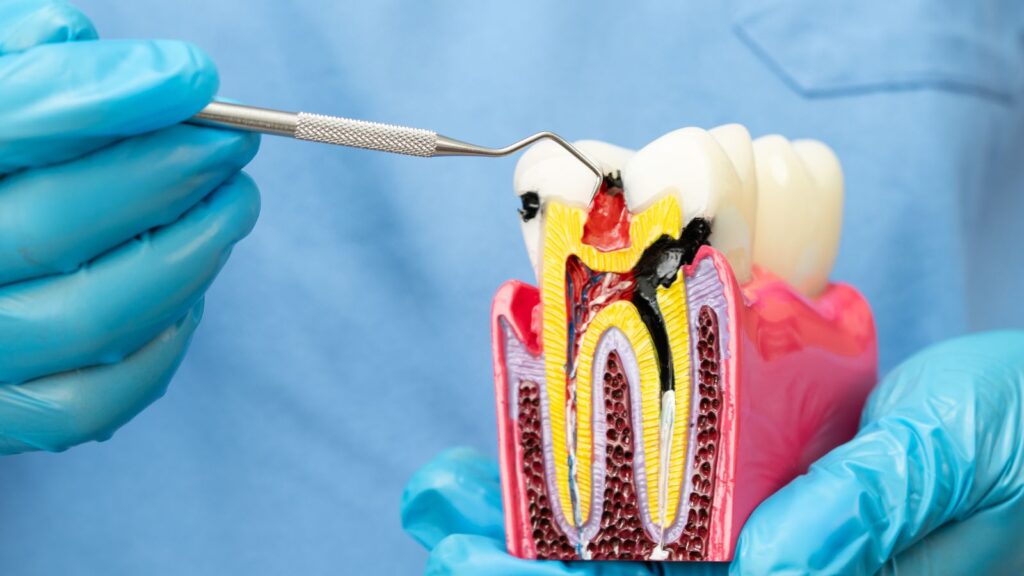
Compromised Bite Function
A poorly planned or fabricated implant restoration can create malocclusion, uneven biting forces, and overload on the implant and neighboring teeth. You may experience pain, chipping of restorations, or accelerated wear of natural teeth when occlusion is not properly balanced.
Functional overload also raises the risk of screw loosening, implant fracture, or bone loss around the implant. Nighttime bruxism or heavy chewing magnifies these problems, turning a single compromised implant into a broader mechanical failure.
Correcting bite problems often requires occlusal adjustments, remanufacture of crowns or bridges, splint therapy, or even removal and replacement of the implant — each step adds time, expense, and treatment complexity.
Aesthetic and Speech Concerns
Cheap implant crowns or poorly matched abutments can result in visible mismatches in tooth shape, color, or gum contour. You may notice dark shadows at the gumline, uneven tooth heights, or unnatural translucency that undermines your smile.
Gum recession and improper emergence profiles change how lips and cheeks support the prosthetic tooth, which can alter pronunciation of certain consonants and affect speech clarity. Minor changes in vertical dimension or tooth position can produce noticeable speech differences.
Addressing aesthetic or phonetic issues may require remaking crowns, soft-tissue grafting, or replacement with more anatomically accurate abutments. Those interventions increase cost and recovery time, and they may not fully restore the original function or appearance without careful, high-quality restorative work.
Choosing Quality Over Cost for Lasting Results
Investing in the right provider, materials, and planning reduces the chance you’ll need corrective work later. Those choices protect your function, appearance, and wallet over decades.
Importance of Experienced Dental Professionals
You should prioritize a clinician with documented implant training and a track record of successful cases. Look for board certifications, continuing education in implantology, and before/after photos that match your case type. Experience matters for implant placement angles, avoiding nerve or sinus injury, and managing limited bone — all factors that affect long-term success.
Experienced teams also coordinate with specialists when needed: oral surgeons for complex extractions, periodontists for grafting, and lab technicians for precise prosthetics. This collaboration reduces surprises during treatment and lowers the risk of revisions, infections, or prosthesis failure that often drive up lifetime costs.
Value of Premium Materials
High-quality implant fixtures, abutments, and crowns use biocompatible titanium or proven zirconia and precise manufacturing tolerances. These materials resist corrosion and integrate with bone more predictably than cheaper alloys or poorly machined components.
Premium prosthetic materials also maintain aesthetics and wear properties longer. For example, a well-fitted ceramic crown paired with a reputable implant system reduces micro-movement and bacterial ingress. That decreases the chance you’ll need replacements, relines, or peri-implantitis treatment later.
Benefits of Comprehensive Treatment Planning
Thorough planning uses CBCT scans, digital impressions, and surgical guides to map bone volume, nerve location, and ideal implant position before you enter the operatory. This reduces intraoperative guesswork and the likelihood of complications that require additional procedures.
A complete plan includes contingency pathways: grafting options, staged loading, and maintenance schedules. It also spells out costs and timelines so you can compare true value rather than headline prices. When planning accounts for your bite, opposing dentition, and esthetic goals, your implants perform better and last longer.