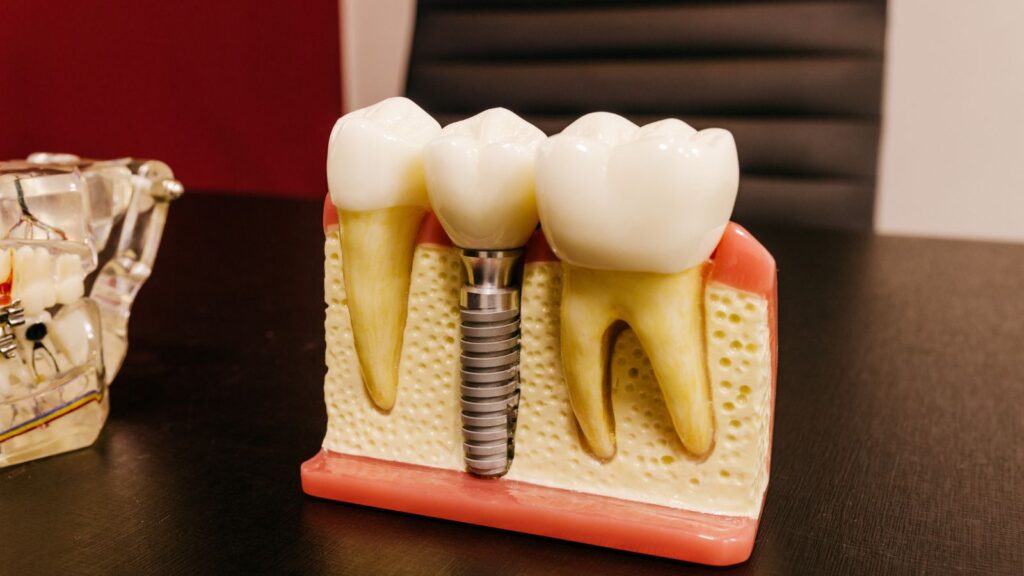
Planning a tooth extraction with future implants in mind can significantly influence both immediate decisions and long-term results. If your goal is to reduce bone loss, avoid additional surgeries, and shorten the timeline to a completed restoration, it’s important to coordinate extraction timing, infection control, and possible bone grafting as part of a comprehensive implant strategy before the tooth is removed.
This article explains how timing, bone quality, and preparatory steps determine whether an implant can be placed immediately, after a brief healing period, or only following additional grafting. You’ll find clear guidance on what to discuss with your provider, how to prepare for surgery, and which factors most impact long-term implant success. Consulting an experienced implant dentist in Evansville, IN early in the process can help you make practical decisions that preserve bone and protect your long-term oral health.
Tooth Extraction With Implants in Mind: Key Considerations
You’ll weigh timing, bone and gum condition, and steps to reduce infection or bone loss. Decisions you make before and after extraction affect how soon an implant can go in and how predictable the outcome will be.
Timing Strategies for Implant Placement
Immediate placement means implanting into the extraction socket during the same visit. You benefit from fewer surgeries and less overall treatment time, but this requires intact socket walls, minimal infection, and good primary stability of the implant.
Early placement occurs 4–8 weeks after extraction. This allows soft-tissue healing while limiting ridge collapse. Choose early placement when minor infection has resolved or when you need modest grafting to support soft tissues.
Delayed placement happens 3–6 months or longer after extraction to allow complete bone remodeling. Use delayed timing if the socket is infected, if you require substantial bone grafting, or if systemic factors (e.g., uncontrolled diabetes, smoking) impair healing.
Assessing Bone and Gum Health
Measure ridge width and height with CBCT or periapical radiographs to determine implant size and the need for grafting. Expect inadequate width or vertical height to require augmentation before or during implant placement.
Evaluate soft-tissue quality: thin or scarred gingiva increases recession risk. Consider connective tissue grafts or staged soft-tissue augmentation to improve long-term esthetics, especially in the anterior zone.
Check for active infection and periodontal disease. Treat periodontitis and eliminate periapical infection before implant placement to reduce implant failure risk. Review medical history—osteoporosis medications, bisphosphonates, and smoking influence healing and timing.
Preventing Future Complications
Plan socket preservation when extraction risks ridge collapse. Use bone grafts and a resorbable membrane to maintain ridge contours and simplify later implant placement.
Control infection with targeted antibiotics only when indicated and with proper debridement of the socket. Rely on meticulous surgical technique and primary wound closure when possible to reduce exposure and contamination.
Optimize patient factors: advise smoking cessation for at least several weeks before and after surgery, manage blood glucose in diabetics, and ensure good oral hygiene. Schedule staged follow-ups with radiographs at 4–12 weeks to monitor healing and detect early complications.
Preparing for Tooth Extraction and Implant Placement
You will need a focused evaluation, clear implant selection based on bone and esthetics, and a realistic timeline that may include grafting or immediate placement. These steps determine whether you can get an implant right away or require staged treatment.
Diagnostic Imaging and Evaluation
Your dentist will order a CBCT scan plus periapical and panoramic X-rays to measure bone height, width, and quality at the extraction site. Expect images to show the proximity of the future implant to sinuses, the inferior alveolar nerve, and adjacent tooth roots.
A clinical exam will assess soft tissue health, infection, tooth mobility, and occlusion. Labs or medical clearance may be required if you have uncontrolled diabetes, recent radiation to the head/neck, or are on anticoagulants or bisphosphonates.
Your provider will document periodontal status and any active infection; those issues are often treated before implant placement. Clear diagnostics reduce surprises during surgery and help determine if you need bone grafting, a sinus lift, or a staged approach.
Selecting the Ideal Implant Type
Your bone volume and quality dictate implant diameter, length, and surface treatment. Narrow implants fit sites with limited width; longer implants help when vertical bone is sufficient.
Choose implant platform and connection (internal hex, conical) based on crown type and load expectations. Providers often prefer roughened surfaces and tapered bodies for primary stability in extraction sockets.
If esthetics matter—especially in the anterior—you may select a platform-switching or zirconia abutment to preserve papillae and avoid gray show-through. Discuss immediate versus delayed provisionalization; immediate provisional crowns require high primary stability (usually ≥35 Ncm torque).
Treatment Planning and Timeline
You will receive a plan showing scheduled steps, estimated healing intervals, and contingencies for grafting or infection. Typical timelines:
- Immediate implant: placement at extraction, 3–6 months to final crown if stability and soft tissue permit.
- Early placement: implant 6–12 weeks after extraction to allow soft-tissue healing.
- Delayed placement: implant after 3–6 months when significant bone remodeling or grafting is needed.
If bone grafting or a sinus lift is necessary, add 4–6 months for integration before implant placement. Your plan should list medications (antibiotics, analgesics), smoking cessation guidance, and follow-up visit dates to monitor healing and osseointegration.

Post-Extraction and Implant Success Factors
Successful results hinge on stable bone volume, healthy gums, and timely decisions about implant timing and grafting. You control outcomes by managing infection, choosing appropriate graft materials, and coordinating soft-tissue techniques that preserve or restore contours for the final restoration.
Guided Bone Regeneration and Grafting
When extraction leaves insufficient bone for implant stability, guided bone regeneration (GBR) restores width and height using barrier membranes plus graft material. You’ll commonly see particulate allograft, xenograft, or autograft combined with a resorbable or non-resorbable membrane to exclude soft tissue and allow bone to fill the socket.
Expect a healing period of several months—typically 3–6 months for routine grafts; more for large defects or ridge augmentation. Monitor for membrane exposure and infection; these complications increase failure risk and may require additional surgery. Plan radiographic evaluation (CBCT) before implant placement to verify graft integration and measure available bone for implant diameter and length selection.
Soft Tissue Management
Healthy peri-implant soft tissue preserves aesthetics and seals the implant from bacterial ingress. You should assess gingival biotype, keratinized tissue width, and papilla height before extraction to plan for connective tissue grafts or vestibuloplasty when needed.
Techniques include free gingival grafts to increase keratinized tissue and subepithelial connective tissue grafts to thicken thin biotypes. Timing matters: simultaneous soft-tissue grafting with implant placement can optimize contours when primary closure is achievable; staged grafting may be better when infection or significant inflammation exists. Track tissue maturation clinically and photographically to guide provisional shaping of the future crown emergence profile.
Immediate vs. Delayed Implant Placement
Immediate implant placement (same day as extraction) can preserve bone and soft-tissue architecture, but it requires an intact socket, absence of acute infection, and adequate primary stability (typically ≥35 Ncm). You should use gap grafting and provisionalization strategies to support the buccal plate and soft tissue when choosing immediate placement.
Delayed placement (healed site, often 3–6 months) offers greater predictability when sockets are infected, bone is deficient, or soft-tissue repair is required. Early placement (4–8 weeks) provides a middle ground: soft tissue begins to heal while some bone remodeling remains manageable. Base your timing on CBCT findings, probing depths, and ability to achieve primary stability; document decisions and contingency plans for grafting or staged approaches.