Varicose veins are common, especially among people who sit or stand for long hours—making them a practical concern for online business owners, marketers, and agency teams who spend extended time at a desk. While some varicose veins are purely cosmetic, others may indicate underlying venous insufficiency that can lead to pain, swelling, skin changes, or even ulcers if left untreated.
This guide explains what varicose veins are, when to seek professional care, which treatment options are proven to work, and which approaches tend to fall short. It also offers practical tips on how to choose the right provider, such as a reputable Central Austin vein clinic, so readers can make informed healthcare decisions without sacrificing time, productivity, or focus on their business goals.
What are Varicose Veins and Who Gets Them?
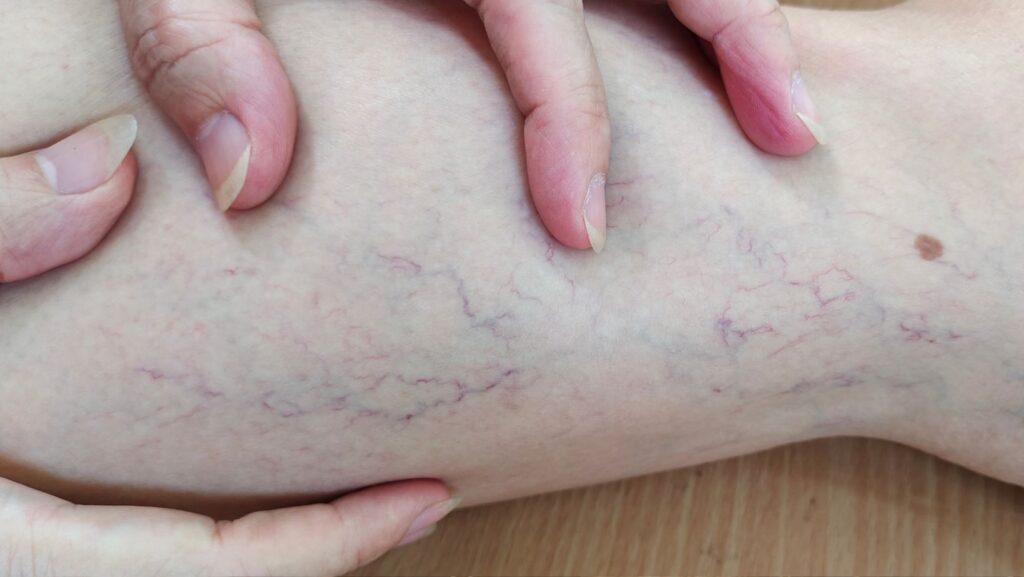
Varicose veins are enlarged, twisted superficial veins that most often appear in the legs. They result from weakened or damaged venous valves that normally keep blood flowing toward the heart. When valves fail, blood pools, veins dilate, and the characteristic bulging, blue or purple veins become visible.
Who gets them? Varicose veins affect roughly 20%–30% of adults worldwide, with higher rates in women and older adults. Risk factors include prolonged standing or sitting, pregnancy, obesity, a family history of venous disease, hormonal factors, and prior leg injuries or deep vein thrombosis. For people running online businesses or agencies, long hours at a desk can increase risk if not balanced with movement and breaks.
Not all varicose veins are the same. Some reflect superficial cosmetic issues: others indicate chronic venous insufficiency (CVI), where deeper venous pathways are compromised. Assessment by a vein specialist helps determine the type and extent of disease, which guides appropriate treatment.
When to Seek Treatment
Deciding when to treat varicose veins depends on symptoms, complications, and personal priorities. The following subsections break down practical triggers for evaluation or intervention.
Symptoms that Warrant Evaluation
Any of these symptoms should prompt an evaluation:
- Aching, throbbing, or burning pain in the legs that worsens after standing.
- Heaviness or fatigue in the legs, especially late in the day.
- Persistent swelling in the ankles or lower legs.
- Cramping or restless legs during the night.
If symptoms interfere with work or daily life, for example, making it hard to stand during meetings or causing restless nights that reduce daytime productivity, a consultation is reasonable. Many people assume varicose veins are only cosmetic, but symptomatic veins often respond well to treatment.
Red Flags and When to Seek Urgent Care
Seek prompt medical attention if any of the following occur:
- Sudden, severe leg swelling or pain that comes on quickly.
- Signs of infection over a vein (increasing redness, warmth, fever).
- Skin ulceration or open sores near the ankle.
- Sudden shortness of breath or chest pain (rarely, blood clots in deep veins can travel to the lungs).
These may indicate deep vein thrombosis (DVT), cellulitis, or venous ulcers, conditions that require urgent assessment and treatment.
Cosmetic Versus Medical Indications for Treatment
Treatment goals fall into two categories:
- Cosmetic: Improve the appearance of visible veins. Many patients choose minimally invasive options or sclerotherapy for spider veins and small varicosities.
- Medical: Relieve pain, reduce swelling, heal or prevent ulcers, and treat underlying venous reflux.
A duplex ultrasound is the standard diagnostic test to map reflux and guide therapy. Even when the primary driver is cosmetic, ruling out significant reflux ensures the selected approach is effective and durable.
Proven Treatments and How They Work
Modern venous care emphasizes minimally invasive methods that address the underlying faulty veins rather than just trimming or removing visible branches. The subsections below summarize commonly used, evidence-based treatments.
Compression Stockings and Conservative Care
Compression stockings (20–30 mmHg or 30–40 mmHg, depending on severity) improve symptoms by supporting venous return and can reduce swelling and pain. Conservative care also includes leg elevation, weight management, regular walking or movement breaks, and avoiding prolonged standing or sitting.
Compression is often the first-line measure and may be sufficient for mild disease or for patients delaying procedural therapy. But compression doesn’t repair faulty valves; it manages symptoms.
Sclerotherapy (Liquid and Foam)
Sclerotherapy involves injecting a chemical sclerosant into a vein to irritate and collapse it. Liquid sclerotherapy works well for small varicose veins and spider veins: foam sclerosants can treat larger trunks. Over weeks to months, the treated vein scars and is reabsorbed.
Sclerotherapy is quick, usually done in-office, and has good cosmetic and symptomatic outcomes. Multiple sessions may be needed, and compression afterward speeds healing and improves results.
Endovenous Thermal Ablation (Laser)
Endovenous laser ablation (EVLA) uses heat from a fiber inserted into the vein to seal it shut. It treats the source of reflux (often the great saphenous vein) with high success rates (>90% occlusion at 1 year in many series). Recovery is typically quick; patients walk immediately and resume normal activities within days. Minor bruising, temporary nerve irritation, or tightness are common short-term effects.
Radiofrequency Ablation (RFA)
RFA uses radiofrequency energy to heat and close the vein. Outcomes and recovery mirror EVLA, and choice between RFA and EVLA often depends on provider preference, vein anatomy, and available equipment. Both dramatically reduced the need for open surgery compared with historical approaches.
Ambulatory Phlebectomy / Microphlebectomy
For bulging surface veins, ambulatory phlebectomy removes segments through tiny incisions using specialized hooks. It’s often combined with ablation of the underlying refluxing vein to prevent recurrence. Performed under local anesthesia, it provides immediate cosmetic improvement with low downtime.
Lifestyle, Medications, and Adjunct Therapies
Lifestyle modification, regular movement, leg elevation, weight control, and smoking cessation complement procedural care. Medications like venoactive drugs (e.g., micronized purified flavonoid fraction) can reduce symptoms in some patients but aren’t substitutes for definitive treatment when reflux is present. Physical therapy and targeted exercises also help with recovery and prevention.
Treatments that Often Fall Short
Not all marketed remedies deliver meaningful or lasting results. The two subsections below clarify common pitfalls and when conservative care is appropriate.
Topical Creams, Alternative Remedies, and Exercise Alone
Topical creams and herbal supplements might soothe aching legs temporarily, but they do not correct venous reflux or eliminate bulging varicosities. Exercise improves circulation and weight control, but won’t close refluxing veins. Similarly, compression stockings control symptoms but don’t cure the underlying problem. Patients seeking permanent reduction of visible veins or relief from significant symptoms should consider evidence-based procedures (sclerotherapy, ablation, phlebectomy) guided by ultrasound.
When Conservative Care is Appropriate Versus Insufficient
Conservative care is appropriate when symptoms are mild, during pregnancy (many providers defer invasive treatments until after delivery), or when patients prefer to avoid procedures. It’s insufficient when there’s significant reflux on duplex ultrasound, recurrent ulcers, progressive skin changes, or when symptoms substantially limit daily function or work performance.
Choosing a Provider and What to Expect From Treatment
Selecting an experienced vein specialist (venous surgeon, vascular surgeon, or interventional radiologist with venous expertise) reduces risk and improves outcomes. For professionals balancing business responsibilities, picking a provider who offers efficient evaluation and streamlined scheduling is time well spent. The subsections below summarize practical considerations during selection and treatment.
Questions to Ask a Vein Specialist
When consulting, patients should ask:
- What’s causing my varicose veins (results of duplex ultrasound)?
- Which treatment do you recommend and why?
- What are the risks and expected recovery time?
- How many procedures like this have you performed?
- Will I need compression afterward, and for how long?
- What are the expected costs and insurance coverage?
Clear answers to these questions help set realistic expectations and streamline decision-making for busy professionals.
Typical Treatment Timeline, Recovery, and Costs
Most modern treatments are outpatient and completed in under an hour. Typical timeline:
- Day of: In-office procedure under local anesthesia: patient walks immediately after.
- First week: Some bruising, soreness, and tightness: compression for 1–2 weeks is commonly recommended.
- 1–4 weeks: Return to routine work; strenuous exercise may be delayed 1–2 weeks.
- 3–6 months: Cosmetic and symptomatic improvements consolidate; follow-up duplex may confirm closure.
Costs vary by region and procedure. Ablation and phlebectomy can cost several thousand dollars: sclerotherapy is often less per session but may require multiple visits. Many insurance plans cover treatment when medical indications (pain, swelling, ulcers, documented reflux) are present. Patients should verify benefits before scheduling.
Prevention and Long-Term Self-Care
Prevention focuses on reducing venous pressure and protecting vascular health. The following subsections give practical, business-friendly strategies.
Practical Daily Measures and Work/Lifestyle Modifications
Simple habits that fit into a busy schedule:
- Move, set a timer to stand and walk for 5 minutes every hour.
- Elevate feet for short periods during breaks to reduce pooling.
- Wear compression stockings during long travel or prolonged standing.
- Optimizing ergonomics, a sit-stand desk helps alternate positions.
- Maintain a healthy weight and include leg-strengthening exercises.
These steps reduce symptom progression and support recovery after procedures.
When to Schedule Follow-Up and Ongoing Monitoring
Typical follow-up includes a visit and duplex ultrasound at 4–12 weeks post-procedure and periodic checks thereafter if symptoms recur. Patients with chronic venous disease benefit from annual or biennial monitoring to catch new reflux early. For busy entrepreneurs, scheduling follow-ups alongside other routine healthcare appointments ensures continuity without disrupting operations.
Conclusion
Varicose veins range from cosmetic nuisances to medical problems that impair comfort and function. Treatment decisions should be guided by symptoms, duplex ultrasound findings, and patient priorities. Evidence-based, minimally invasive treatments, such as sclerotherapy, endovenous ablation, and phlebectomy, reliably address the root causes of reflux while offering quick recovery suitable for professionals with limited downtime. Conservative care and lifestyle adjustments remain important adjuncts, but they rarely replace definitive therapy when significant reflux or complications exist.
For online business owners and agency professionals, timely evaluation prevents small problems from becoming disruptive. Asking the right questions, choosing an experienced vein specialist, and pairing procedural care with practical self-care will deliver the best outcomes, so they can get back to running their business with fewer leg worries.